Health
JUST-IN: Diphtheria Hits King’s College, Parents Blame Poor Hygiene
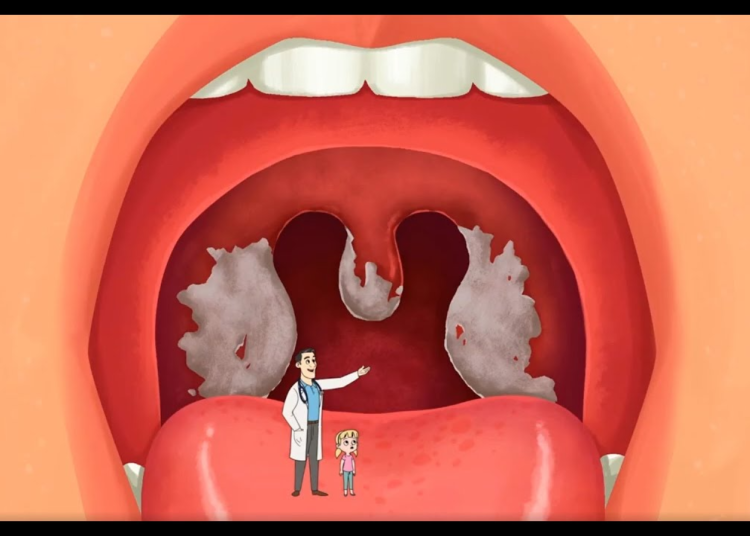
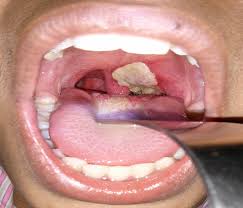
A diphtheria outbreak at King’s College, Lagos (KCL), has sparked outrage among parents, who blamed poor sanitation and inadequate hygiene for the spread of the deadly bacterial infection.
The outbreak, which has resulted in multiple hospitaliSations and one confirmed fatality among students, has prompted the Lagos State Government to activate its Emergency Operations Centre (EOC) to contain the situation.
Parents have long raised concerns about the deteriorating condition of the school’s facilities, citing issues such as unsanitary toilets, poor waste management, and unhygienic food preparation.
Many believed these conditions created a breeding ground for infections, making students vulnerable to diphtheria and other illnesses.
A concerned parent, speaking anonymously, questioned why the school had initially downplayed the situation despite clear signs of a looming outbreak.
“If hygiene wasn’t an issue, why are students suddenly wearing nose masks? Why were some rushed to LUTH for treatment? This could have been prevented if the school took health and sanitation seriously,” she said.
Reports suggest that students had shown symptoms of diphtheria weeks before the official confirmation, with some parents claiming their children were diagnosed in external hospitals.
However, attempts to raise these concerns within the school’s Parent-Teacher Association (PTA) were reportedly dismissed.
Following the outbreak, King’s College management issued consent forms requesting parents’ approval for their children to receive diphtheria vaccinations.
The immunization campaign, carried out in collaboration with the Lagos State Primary Health Care Board, aims to boost immunity among students and prevent further spread.
The Lagos State government, reacting swiftly, activated its Emergency Response Committee.
Commissioner for Health, Prof. Akin Abayomi, confirmed that the index case was a 12-year-old student who reported to the school’s clinic on February 22 with a sore throat and fever.
“He was referred to LUTH, where he received antibiotics and diphtheria antitoxin serum.
However, despite medical intervention, he succumbed to severe myocarditis—a known complication of diphtheria toxin—on March 6.
At the time of his death, 34 close contacts were already under medical observation. Of these, 14 students developed symptoms and were transferred to LUTH for screening.
Twelve were confirmed to have early-stage diphtheria and placed on immediate treatment,” the Commissioner disclosed.
Abayomi averred that the state government has now launched a mass vaccination campaign for students at both the Victoria Island Annexe and the Main School in Igbosere, extending immunization efforts to teachers and healthcare providers, adding that a health inspection at King’s College revealed gaps in infection prevention and control (IPC) measures, which officials have vowed to address immediately.
“To curb further spread, the government is distributing diphtheria awareness materials across schools and hospitals in Lagos.
A public health advisory is also being prepared to educate residents on symptoms, prevention, and early treatment.
“With nearly 500,000 doses of diphtheria vaccines available, health authorities, including the World Health Organization (WHO), Nigeria Centre for Disease Control (NCDC), and the National Primary Health Care Development Agency (NPHCDA), are collaborating to contain the outbreak and prevent future occurrences, he stated.
Parents, however, insisted that the root cause of the problem must be addressed. Many were calling for urgent government intervention to improve water supply, sanitation, waste management, and healthcare facilities in the school.
One disraut mother, whose son was hospitalised for over a week, lamented the poor conditions students endure. “This is not just about diphtheria.
The entire school environment is unhealthy.
If nothing changes, we will keep seeing outbreaks of diseases that could have been prevented with basic hygiene,” she said.
As the State Emergency Operations Centre continues to monitor the evolving situation, Commissioner Abayomi has urged Lagosians to prioritise hygiene, avoid crowded environments, and seek immediate medical attention if experiencing diphtheria symptoms.
He reassured the public that the outbreak is under control, and proactive measures will continue to protect students and prevent future health crises.
Health
WHO Declares Emergency As Ebola Kills 88 In Congo
Early symptoms include fever, muscle pain, fatigue, headache, and sore throat, and are followed by vomiting, diarrhoea, a rash, and bleeding.
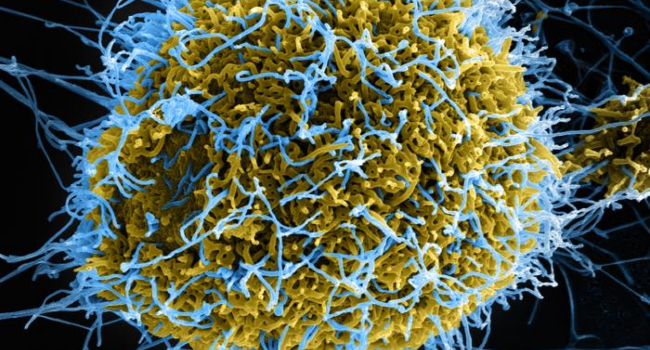
• Ebola
The World Health Organization (WHO) has declared the latest Ebola outbreak in the DRC and neighbouring Uganda a “public health emergency of international concern”.
The outbreak, originating in eastern DRC’s Ituri province, which has seen around 246 suspected cases, involves the rare Bundibugyo strain of Ebola.
The variant has no approved vaccine or treatment.
Health authorities said the outbreak poses a high regional risk because infections have already been detected in Uganda, and cases linked to the outbreak have reached Congo’s capital, Kinshasa, and killed 88 people.
The WHO, however, stopped short of declaring a pandemic, saying it did not meet the necessary criteria.
The United Nations agency advised countries against closing borders or restricting trade.
Early symptoms include fever, muscle pain, fatigue, headache, and sore throat, and are followed by vomiting, diarrhoea, a rash, and bleeding.
Health
National Data Repository Index Numbers of patients currently on treatment for HIV in Nigeria as at May 13, 2026
Benue: 195,305
- Akwa Ibom: 158,201
- Lagos: 135,918
- Rivers: 90,055
- Nasarawa: 65,996
- FCT: 62,627
- Kaduna: 58,576
- Cross River: 57,765
- Enugu: 55,478
- Delta: 52,475
- Taraba: 51,840
- Abia: 50,038
- Imo: 47,863
- Plateau: 46,618
- Anambra: 46,602
- Adamawa: 42,074
- Kano: 41,093
- Kogi: 37,301
- Oyo: 33,133
- Niger: 33,057
- Ogun: 31,822
- Bauchi: 29,745
- Edo: 29,256
- Gombe: 28,037
- Osun: 25,018
- Borno: 24,527
- Ondo: 22,455
- Kebbi: 20,803
- Bayelsa: 19,549
- Katsina: 18,682
- Ebonyi: 15,474
- Kwara: 14,997
- Jigawa: 14,302
- Zamfara: 13,813
- Ekiti: 12,356
- Yobe: 10,716
- Sokoto: 10,511 Total: 1.70m
Health
FG to Launch Mega Agro-Industrial Livestock HUB in Abuja

The Federal Government has reaffirmed its commitment to the establishment of an Agro-Industrial Business Hub and Mega Livestock Processing Facility in the Federal Capital Territory, Abuja.
The Minister of Livestock Development, Idi Mukhtar Maiha, gave the assurance during a high-level strategic meeting involving the Federal Ministry of Livestock Development, ABIS Group and the Livestock Productivity and Resilience Support Project (LPRES) in Abuja.
The Minister stated that the Ministry would work closely with ABIS Group, LPRES and other stakeholders to ensure the smooth take-off and successful implementation of the project. He explained that the engagement followed Nigeria’s participation in an international training programme on pastoral market access and inclusive contracting models held in Addis Ababa, Ethiopia.
According to the Minister, the training, organised under the auspices of the African Union Interafrican Bureau for Animal Resources and the African Pastoral Market Development Platform, provided valuable insights into strengthening livestock value chains, improving market systems and promoting quality assurance mechanisms across Africa.
Leader of the ABIS delegation, Ambassador Emmanuel Usman, commended the Ministry for facilitating the group’s participation in the training programme, which brought together delegates from Somalia, Botswana, Ethiopia and Kenya.
Also speaking, LPRES National Coordinator, Sanusi Abubakar, appreciated the Minister for supporting collaboration and inclusiveness in the livestock sector.
The General Manager of ABIS Group, Mr. Kujo Reigans, highlighted key lessons from the training, including the need for a unified quality assurance system, structured outgrower schemes and improved access to funding opportunities through the Development Bank of Nigeria.
He stated that these measures would enhance efficiency, traceability and competitiveness within Nigeria’s livestock industry.
The ABIS team also raised concerns over visa bottlenecks affecting expatriates working on the Abuja Mega Livestock Processing Facility project, calling for streamlined visa processes to ease project implementation and support the timely delivery of the agro-industrial hub in the FCT.
-

 Business3 days ago
Business3 days agoFemi Otedola earmarks $100 million for Dangote Refinery’s IPO
-

 Politics3 days ago
Politics3 days agoAtiku Appears Before ADC Presidential Screening Panel
-

 Politics3 days ago
Politics3 days agoGov Fubara withdrawals from governorship race
-

 Entertainment3 days ago
Entertainment3 days agoWizkid Becomes First African Artist to Surpass 11 Billion Spotify Streams
-

 Entertainment3 days ago
Entertainment3 days ago‘God Took Him’ — Singer Niniola Announces Death of Husband Michael Ndika
-

 Politics2 days ago
Politics2 days ago2027: Natasha emerges PDP Kogi central ticket
-

 Politics3 days ago
Politics3 days agoTinubu Doesn’t Trust Me Because I’m Igbo’ — Cubana Chief Priest Opens Up on APC Reps Ticket Loss’
-

 News2 days ago
News2 days agoNYSC warns against night travel as 2026 Batch B Stream I orientation begins June 10